Sleep materials
Below you will find an overview of various materials for download that can be used in clinical practice for further evaluating sleep problems. The Holland Sleep Disorders Questionnaire (HSDQ), developed by Gerard Kerkhof and colleagues (Kerkhof et al., 2013), can be used in the diagnostic phase and provides information if people are suspected of specific sleep disorders such as sleep apnea, resless legs, circadian rhythm sleep disorder etc. Note these results should not be considered ‘diagnostic’ but merely an indication – or red-flag – to investigate such sleep problems in more detail. The Pittsburgh Sleep Quality Index (PSQI) is a self-report questionnaire that evaluates various aspects of sleep quality and can be used for repeated administrations to track progress and treatment effects on sleep. Furthermore, the sleep-wake diary can be used by clients to systematically keep track of their sleep across a week. Finally, for further reference, on the right we included a sleep guideline with recommendations for bedtimes and optimal sleep duration across the lifespan, which was derived from various sources as included in the graphic and references below. For further information also see a recent review on the role of sleep and the circadian system in the etiology of ADHD here, or a Dutch summary on the role of light sleep and tablets on concentration or English see here.
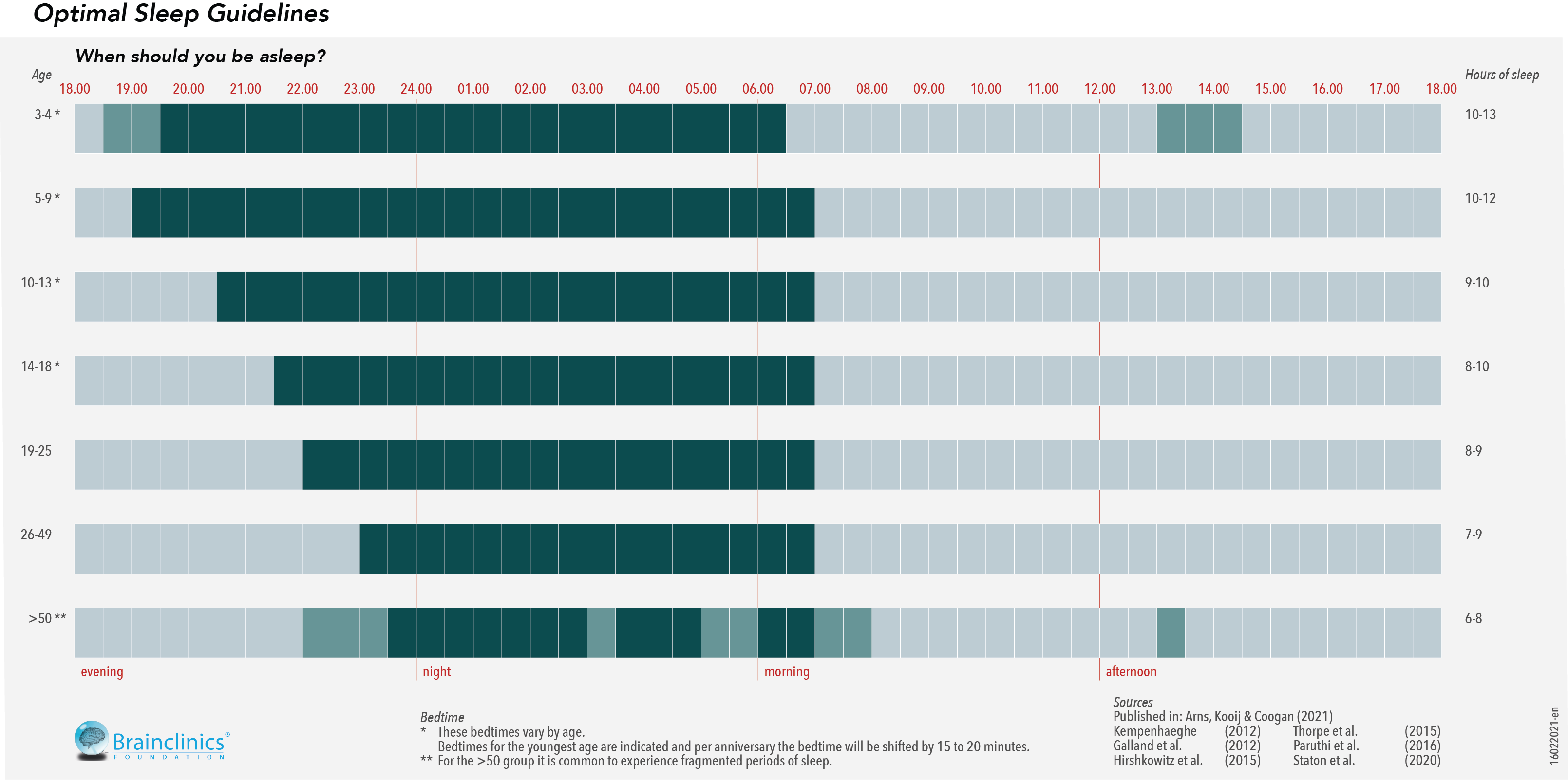
Figure 1: Recommended age-appropriate bedtimes and wake-up times, as well as number of hours sleep per night (right). Note that dark shading implicates sleep times, and the lighter colors in the youngest (3-4 yrs.) and oldest (>50 yrs.) age groups indicate exchangeable times, i.e. when someone naps during the day. For the >50 yrs. age group the lighter colors further indicate higher occurrences of fragmented sleep that are more common at those ages. Also note that if sleep offset times are different, e.g. 8 AM instead of 7 AM, that other times shift along as well. These recommendations have been derived from recommendations and guidelines from the American Academy of Sleep Medicine (AASM), the Kempenhaeghe Sleep Clinic, and the latest systematic reviews and meta-analyses on sleep duration and napping, see references below.
Also see: Martijn Arns, J.J. Sandra Kooij, Andrew N. Coogan (2021)
Review: Identification and Management of Circadian Rhythm Sleep Disorders as a Transdiagnostic Feature in Child and Adolescent Psychiatry;doi.org/10.1016/j.jaac.2020.12.035
Downloads
Further reading
- Martijn Arns, J.J. Sandra Kooij, Andrew N. Coogan (2021)
Review: Identification and Management of Circadian Rhythm Sleep Disorders as a Transdiagnostic Feature in Child and Adolescent Psychiatry;doi.org/10.1016/j.jaac.2020.12.035 - Kerkhof, G., Geuke, M., Brouwer, A., Rijsman, R., Schimsheimer, R., Kasteel, V. (2013). Holland Sleep Disorders Questionnaire: a new sleep disorders questionnaire based on the International Classification of Sleep Disorders‐2 Journal of Sleep Research 22(1), 104-107. doi:10.1111/j.1365-2869.2012.01041.x
- Hirshkowitz M, Whiton K, Albert SM, et al. National Sleep Foundation’s sleep time duration recommendations: methodology and results summary. Sleep Heal. 2015;1(1):40-43. doi:10.1016/j.sleh.2014.12.010
- Galland BC, Taylor BJ, Elder DE, Herbison P. Normal sleep patterns in infants and children: A systematic review of observational studies. Sleep Med Rev. 2012;16(3):213-222. doi:10.1016/j.smrv.2011.06.001
- Paruthi S, Brooks LJ, D’Ambrosio C, et al. Consensus Statement of the American Academy of Sleep Medicine on the Recommended Amount of Sleep for Healthy Children: Methodology and Discussion. J Clin Sleep Med. 2016;12(11):1549-1561. doi:10.5664/jcsm.6288
- Staton S, Rankin PS, Harding M, et al. Many naps, one nap, none: A systematic review and meta-analysis of napping patterns in children 0-12 years. Sleep Med Rev. Published online 2019:101247. doi:10.1016/j.smrv.2019.101247