ADHD, iPads, sleep and concentration problems: Shedding new light on ADHD?
ADHD sleep LED light
At schools, the idea still prevails that easily distracted children and children with ADHD should not be seated too close to the window, since they might be distracted by what is happening outside. ADHD is often associated with difficulties in attention and higher controlling functions in the brain (executive functioning). Are these symptoms truly the core issue in ADHD, or could there be a different underlying cause? In this article we discuss this in further detail and show that some easily distracted children might be better off sitting closer to the window.
Most parents are aware that no two children are the same. Accordingly, we know that no two children with ADHD are the same, even though they share the same “diagnosis”. Oddly enough, this principle is only recently beginning to get accepted in psychiatry. Over the last few years, it has become increasingly clear that the treatment of ADHD with psychostimulants such as Ritalin only has sustained effects beyond 2 years in 30-40% of the patients. Recent insights of this kind make it clear that we can assume that there can be various causes of ADHD, and that – from a neurobiological perspective – it is not a homogeneous disorder that logically therefore cannot be remedied with one homogeneous treatment for everyone. The development in which diversity in possible causes that can explain “ADHD behavior” is the starting point, and in all likelihood requires different treatment approaches depending on the cause, is often referred to as ‘Personalized Medicine’ or ‘Precision Medicine’. Brainclinics specializes in the above-mentioned “Personalized Medicine” for ADHD, using applied brain research such as EEG research, neuropsychological research, and innovative new treatments such as neurofeedback in the treatment of ADHD and magnetic brain stimulation (rTMS for depression). Within Brainclinics, we have conducted various studies over the past 10-15 years into subgroups within ADHD. These studies show that there is a subgroup of children with ADHD, where the brain activity (as measured with the Electroencephalogram, or EEG) shows clear signs of fatigue or drowsiness. This subgroup appears to be the same group that responds well to medication (including Ritalin) and neurofeedback. Conceptually it can be understood that a stimulant (psychostimulant) has a beneficial effect on signs of fatigue.
We have recently found evidence that ‘methylphenidate’ (the active ingredient in, for instance, Ritalin and Concerta) not only stimulates, but also sensitizes the biological clock. The biological clock is strongly influenced by daylight. We therefore examined the annual seasonal variation in concentration before and after treatment with methylphenidate in a large-scale worldwide drug study. We found that patients treated with a low dose during a shortening of days (especially in the fall) showed the same concentration improvement as patients treated with a high dose. This effect disappeared again with the days getting longer: Only during lengthening of days (especially in the spring) patients treated with a high dose showed a greater improvement in their concentration compared to those receiving a low dose.
ADHD sleep LED light
Over the last 10 years, we have also focused on non-pharmacological treatment and have extensively investigated the use of neurofeedback, a treatment in which direct feedback is given on brain activity, as a treatment for ADHD. Based on this, a learning process takes place where clients intend to learn how to switch certain brain networks on and off. This often results in an improvement in sleep and an improvement in ADHD complaints such as attention and impulsiveness. Unfortunately, some parties are ‘over-claiming’ all kinds of uses of neurofeedback. When consulting the internet, one would almost think that neurofeedback is a panacea for everything. In addition, there is a wide variety in “neurofeedback methods” applied, of which some are well investigated with clear indications that they have an effect in the treatment of ADHD (Arns, Heinrich & Strehl, 2013, follow up meta-analyse referentie). However, there are also many questionable methods, which have not been investigated at all, claiming that it helps with ADHD and many other conditions such as OCD, burnout, addiction etc. In summary, one should have relatively most confidence in therapists who claim less (e.g., who limit themselves to the treatment of ADHD). And, just like regular ADHD treatment should be carried out by a trained psychologist, the same should apply to neurofeedback treatment (and this is often not the case).
In working with neurofeedback and ADHD, we have noticed for years that the most common “side effect” reported by patients, was that they slept better, even when no sleeping problems were apparent. Based on this fact and other scientific studies explaining this “sleep enhancing effect” of neurofeedback, we published a model that relates sleep problems to symptoms in the ADHD spectrum, such as concentration problems, impulsivity, etc. (Arns & Kenemans, 2012).
What does this relationship between sleep problems and ‘symptoms of ADHD’ entail?
To understand this better, it is important to distinguish between ‘sleep deprivation’, i.e. a full night without sleep, of which we know that it substantially affects daily functioning, and ‘sleep restriction’. Sleep restriction means, for example, sleeping half an hour or an hour less. It is known that, in the long term, this results in impaired attention functioning and in the typical ‘drowsiness’ brain activity as described above. If adults are requested to sleep 6 instead of 8 hours per night for two consecutive weeks, their attention and concentration will gradually decline from day to day. When asked about their functioning after two weeks of sleep restriction, they will report no complaints. However, when attention is measured objectively, it will become clear that their functioning is at the same level as it would have been after two nights of full sleep deprivation! The big difference of sleep restriction as compared to sleep deprivation lies in the fact that a person with long-term sleep restriction needs the same number of nights of “normal 8 hours of sleep” to function at the level before the sleep restriction. In other words, sleeping-in on the weekends is not sufficient to recover from the loss of sleep during the week. Furthermore, large-scale studies have shown that sleep duration is positively correlated with executive functioning and school functioning, and negatively correlated with externalizing behavior (disobedient, disturbing, hyperactive and impulsive behavior, etc.). Also, several studies have shown that healthy children exposed to sleep restriction will display more ‘ADHD-like’ behavior.
In this perspective it is also interesting to know that children nowadays sleep an average of 1 hour and 15 minutes less than a 100 years ago. More objectively, studies using EEG have substantiated this trend further and reveal that, during the last ten years, healthy children’s brain activity is showing more signs of drowsiness. Considering this, it becomes clear that sleep indeed plays a fundamental role in our daily functioning, and that it can indeed play a role in the development of complaints that are also seen in ADHD. In addition, these trends may partly explain the increase of concentration problems and increased prevalence of ADHD in our society.
It is known that various sleep disorders are more common among children with ADHD, such as Restless Legs Syndrome (RLS) and sleep-breathing problems or sleep apnea (manifested through snoring, and a temporary cessation of breathing during sleep). Interestingly, it was observed in several studies that treating sleep disorders such as RLS and sleep apnea resulted in a substantial improvement in ADHD complaints. Another – more subtle – sleeping problem that occurs in 70-80% of children and adults with ADHD, is sleep onset insomnia (SOI), i.e. having trouble falling asleep at an age-appropriate bedtime. This is not just a subjective complaint; it can be determined objectively by measuring the release of melatonin (sleep hormone) in the evening, according to Dutch researchers.
ADHD sleep LED light
Delayed melatonin release and the associated difficulty falling asleep is something that is becoming more common. For a better understanding of this matter, it is important to know that, besides rods and cones (responsible for processing visual information), we also have a third receptor in our eyes, the melanopsin receptor. This receptor is sensitive to light, and most specifically to blue light, and plays a role in the regulation of our biological clock. Sunlight has – especially in the morning – a peak in the blue spectrum. Exposure to blue light in the morning – in line with the time of day that sunlight is most intense – is when our biological clock is set. In this way the biological clock functions simultaneously with the 24-hour day-night rhythm of the earth. However, excessive exposure to blue light in the evening (after natural sun set) leads to a suppression of the sleep hormone melatonin, thereby postponing the feeling of being tired resulting in people falling asleep later. The old-fashioned light bulb or incandescent light mainly emits light in the (infra)red spectrum and hardly any light in the blue spectrum. In contrast, modern LED lamps and energy saving lamps (CFL), as well as tablets, computer screens and mobile phones have a peak in the blue spectrum and thus emit a lot of blue light (just look at the ‘blue’ reflection on someone’s face when behind a smartphone or tablet in the dark). Exposure to these light sources at an unnatural time of day, i.e. in the evening, can disrupt our biological clock and make us fall asleep at a later time, hence causing the sleep restriction mentioned above. Interestingly, this effect can be canceled out by increasing blue light exposure in the morning.
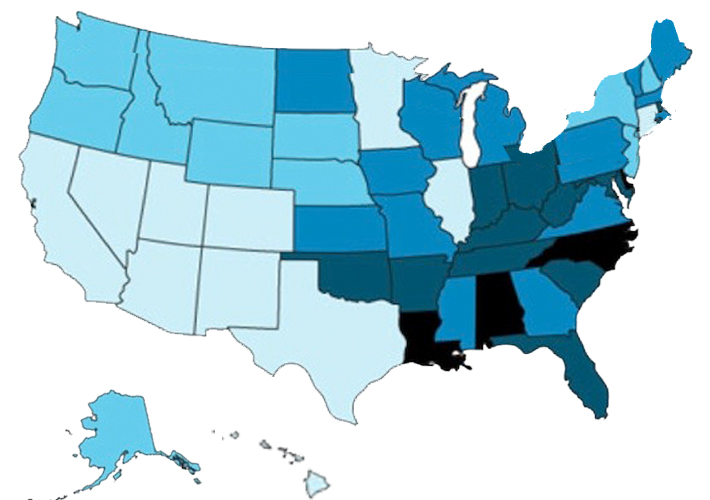
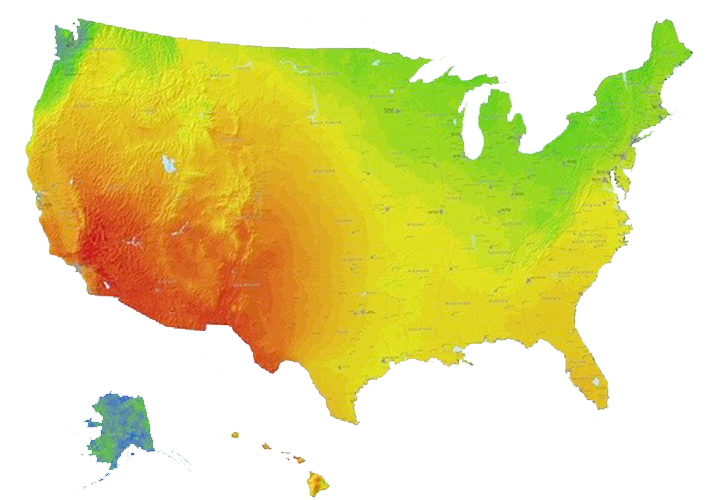
Based on these data, it might be presumed that there is a relationship between exposure to sunlight and the prevalence of ADHD. In 2013, we published a study in Biological Psychiatry where we exactly demonstrated this, (see figure below). This figure shows on the one hand the occurrence – or prevalence – of ADHD in the various states of the US and on the other hand the annual intensity of sunlight. These findings demonstrate that a high intensity of sunlight is associated with a lower prevalence of ADHD. Meanwhile, we have confirmed this relationship in five different datasets, including a dataset with European countries. This relationship explains 34-57% of the prevalence of ADHD in the US and other countries, which is a considerable proportion.
ADHD sleep LED light
The prevalence of ADHD in the various US states can be seen in the blue map, and it is striking that southwest states in particular have a lower incidence of ADHD (CDC, 2003). The colored map overlay shows the intensity of sunlight in the various regions in the US (expressed in KWh/m2/day). This image illustrates the clear overlap between high sunlight intensity (red areas) and low ADHD prevalence (light blue areas).
What is the role of iPads, PCs and LED lamps, and prevention of ADHD?
Now, of course the question arises whether it is recommendable to keep children from using the iPad or computer in the evening. From chronobiology it is known that there is a balance, intense sunlight during the day can advance the sleep phase (and therefore the melatonin peak), while excessive exposure to blue light in the evening has the opposite effect. Higher exposure to blue light during the day – in the form of sunlight – can therefore cancel out the disturbing effect of evening exposure. Our research shows that sufficient exposure to sunlight during the day may have a preventative effect of ADHD. It is our interpretation that a higher prevalence of ADHD is caused by excessive exposure to blue light in the evening, and that a high degree of sunlight during the day cancels out this effect. Banning modern media use in the evening will probably not be realistic. However, free software is available (like F.lux) that will adjust the color settings on the screen of your PC, Mac or iPad, depending on the time of day. Modern smartphones and tablets have this option built-in. Also, LED manufacturers may consider developing LED lights with less affinity in the blue spectrum. Yet, a simple advice may be to just get more daylight exposure in the morning. A project of which we’re still dreaming, is to literally ‘take the roof off’ in schools in the Netherlands, in order to use skylight to provide natural light in the classrooms. The only ‘side effect’ of such an intervention would be a substantial savings on energy costs, thus an ecologically sustainable solution, and possibly a decrease of concentration problems and ADHD. Until that time, simple advices like walking the dog in the morning, walking or cycling to school instead of using a car and, as argued above, providing a seat by the window for that easily distracted child, are a good start.